Varicose veins are a common condition that affects many individuals, particularly as they age. While varicose veins are often harmless and merely a cosmetic concern for some people, they can also cause discomfort and lead to more severe complications. It is important to understand when it is necessary to seek medical treatment for varicose veins to ensure proper care and prevent potential complications. In this article, we will explore the signs and symptoms that indicate the need for medical intervention and discuss the available treatment options.
Introduction
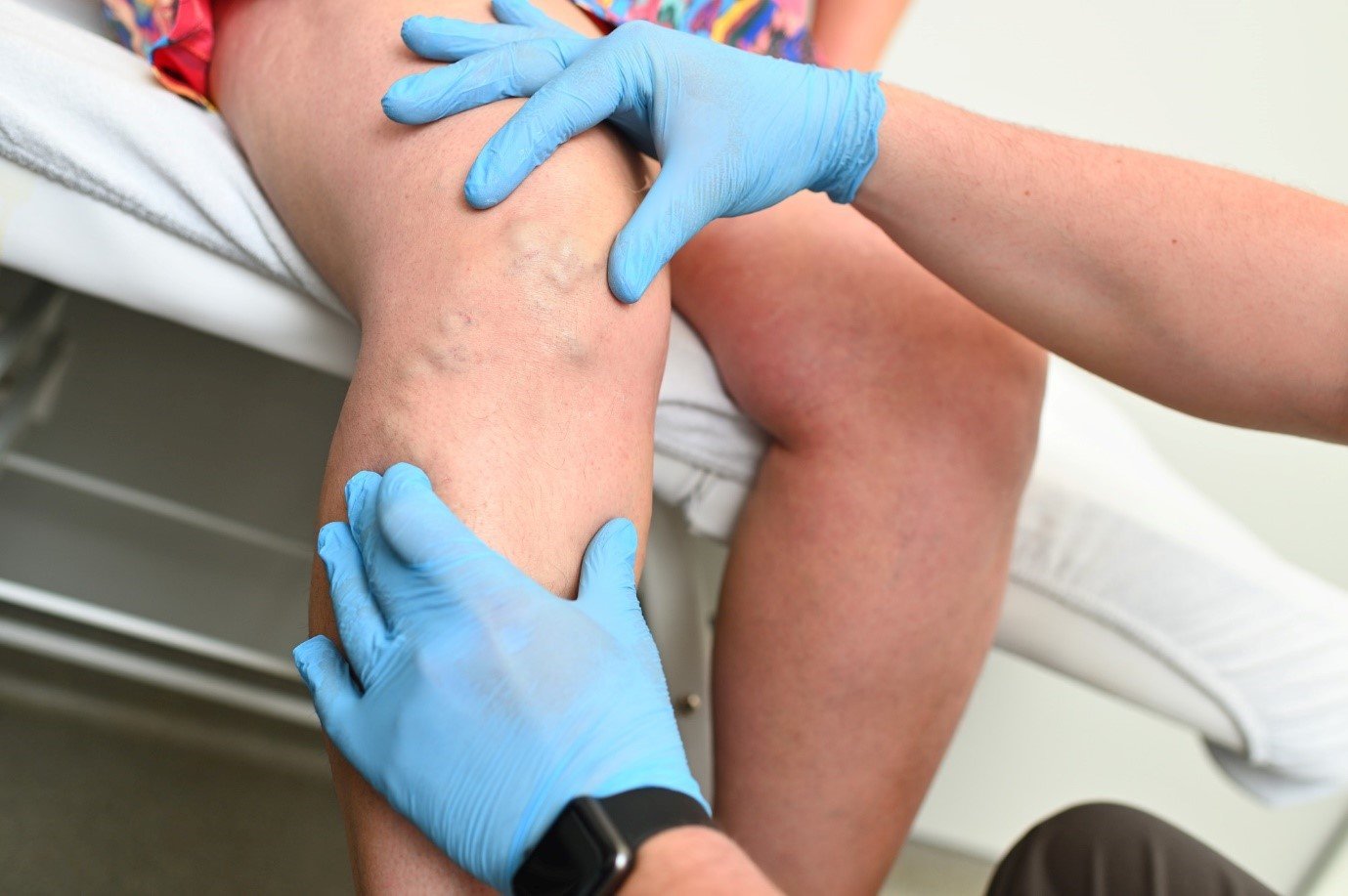
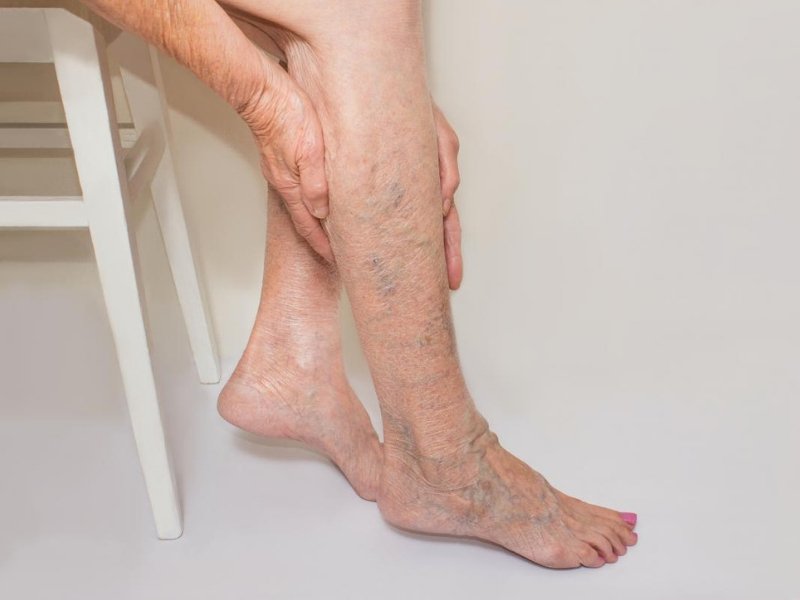
Varicose veins are enlarged, twisted veins that commonly occur in the legs and feet. They can be identified by their bulging appearance and bluish or purplish color. While varicose veins are often a cosmetic concern, they can also cause pain, discomfort, and various complications. It is essential to recognize when medical treatment is necessary to manage the symptoms effectively and prevent further complications.
Understanding Varicose Veins
Varicose veins develop when the valves within the veins fail to function correctly. Normally, these valves help regulate blood flow and prevent backward flow. When they become weakened or damaged, blood can pool in the veins, causing them to stretch, enlarge, and become varicose.
Signs and Symptoms of Varicose Veins
The presence of varicose veins can be accompanied by several noticeable signs and symptoms. These include:
1. Visible veins
Varicose veins are easily visible on the surface of the skin. They often appear twisted, swollen, and raised.
2. Leg pain and discomfort
Individuals with varicose veins may experience pain, aching, or throbbing sensations in the legs. These symptoms may worsen after prolonged periods of standing or sitting.
3. Swelling and heaviness
The affected area around the varicose veins may become swollen and feel heavy, especially at the end of the day or after extended periods of standing.
4. Skin changes
Varicose veins can cause changes in the skin’s appearance. This may include skin discoloration, dryness, itching, or the development of skin ulcers.
When to Seek Medical Attention
While mild cases of varicose veins may not require immediate medical attention, it is important to consult a healthcare professional if any of the following conditions are present:
1. Intense pain or discomfort
If the pain associated with varicose veins becomes severe or interferes with daily activities, it is advisable to seek medical treatment.
2. Swelling and inflammation
If the affected area becomes significantly swollen, red, warm to the touch, or shows signs of infection, medical attention should be sought promptly.
3. Bleeding or ulceration
If the varicose veins start bleeding or develop open sores or ulcers, it is crucial to seek immediate medical care to prevent infection and promote healing.
4. Lifestyle limitations
If varicose veins limit mobility or significantly affect the quality of life, medical intervention can provide relief and improve overall well-being.
Diagnosing Varicose Veins
To determine the appropriate course of treatment, a healthcare professional will conduct a thorough examination and may perform additional diagnostic tests. These may include:
1. Physical examination
A doctor will visually inspect the affected veins and ask about any symptoms or discomfort experienced.
2. Doppler ultrasound
An ultrasound scan is commonly used to evaluate the blood flow within the veins and identify any underlying issues.
Treatment Options
Several treatment options are available to address varicose veins, depending on the severity and specific needs of the individual. These include:
1. Compression stockings
Wearing compression stockings can help improve blood flow and reduce discomfort associated with varicose veins.
2. Sclerotherapy
This procedure involves injecting a solution into the affected veins to cause them to shrink and eventually fade away.
3. Endovenous laser treatment (EVLT)
EVLT is a minimally invasive procedure that uses laser energy to close off the affected veins.
4. Surgical interventions
In more severe cases, surgical procedures such as vein stripping or ligation may be recommended to remove or tie off the affected veins.
Lifestyle Changes and Self-Care Measures
In addition to medical interventions, certain lifestyle changes and self-care measures can help manage varicose veins and reduce discomfort. These include:
- Regular exercise to promote circulation and strengthen leg muscles.
- Maintaining a healthy weight to reduce pressure on the veins.
- Elevating the legs periodically to reduce swelling.
- Avoiding prolonged periods of standing or sitting.
Conclusion
Varicose veins can range from a cosmetic concern to a source of pain and discomfort. Recognizing the signs and symptoms that warrant medical attention is crucial for timely intervention and appropriate management. Various treatment options are available, ranging from conservative measures to more invasive procedures. Consulting with a healthcare professional can help determine the most suitable course of action based on individual needs and preferences.
Frequently Asked Questions (FAQs)
- Can varicose veins go away on their own?
While varicose veins may not disappear completely on their own, certain lifestyle changes and self-care measures can help manage symptoms and prevent their progression.
2. Are varicose veins only a cosmetic concern?
Although varicose veins are often viewed as a cosmetic issue, they can cause pain, discomfort, and potentially serious complications, such as blood clots or ulcers.
3. Are there any natural remedies for varicose veins?
While natural remedies may provide some relief from symptoms, they are unlikely to eliminate varicose veins completely. It is best to consult with a healthcare professional for appropriate treatment options.
4. Can exercise worsen varicose veins?
Regular exercise, particularly low-impact activities such as walking or swimming, can actually improve circulation and alleviate symptoms associated with varicose veins.
5. Is it possible to prevent varicose veins?
While it may not be possible to prevent varicose veins entirely, maintaining a healthy lifestyle, including regular exercise and maintaining a healthy weight, can help reduce the risk and slow their progression.