1. Introduction
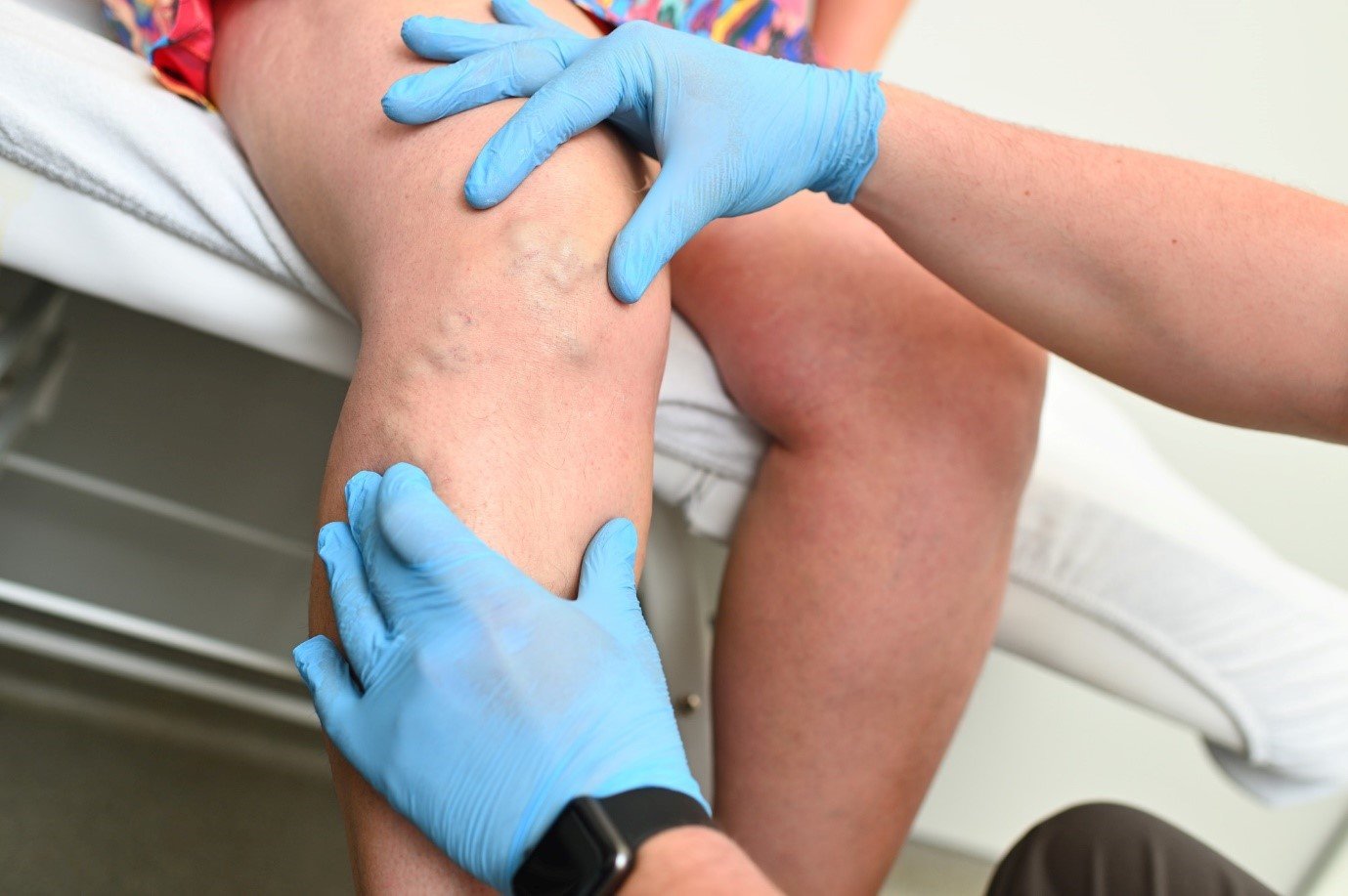
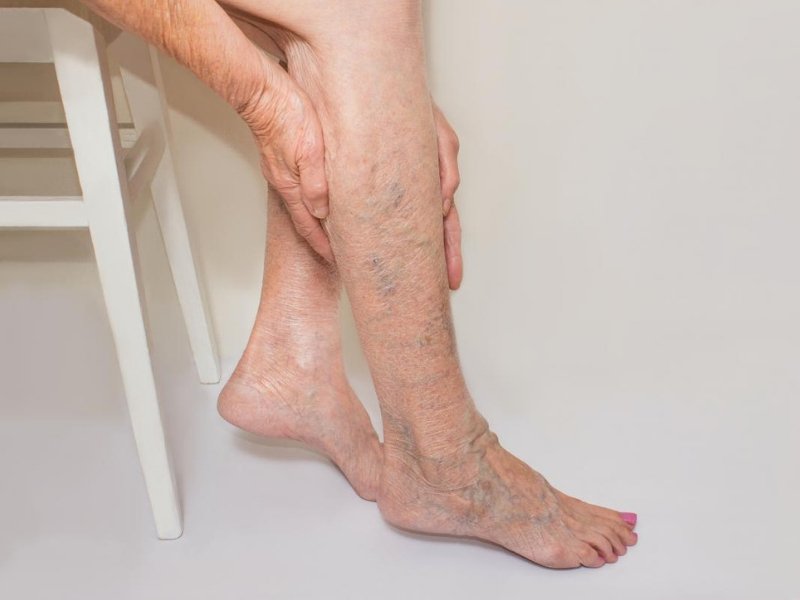
Varicose veins are a common condition characterized by enlarged, twisted veins that often appear on the legs and feet. While lifestyle factors such as obesity, prolonged standing, and lack of physical activity are commonly associated with varicose veins, genetics can also play a significant role in their development. In this article, we will explore how genetics can cause varicose veins and the underlying mechanisms behind this phenomenon.
2. Understanding Varicose Veins
Before delving into the genetic aspects, it is essential to understand the basics of varicose veins. Veins in our body are responsible for carrying deoxygenated blood back to the heart. They have one-way valves that ensure proper blood flow against gravity. When these valves weaken or become damaged, blood can pool in the veins, leading to their dilation and the formation of varicose veins.
3. The Role of Genetics
Research suggests that genetics can influence the development of varicose veins, indicating that some individuals may have a genetic predisposition to the condition. While not everyone with a family history of varicose veins will develop them, having certain genetic factors can increase the likelihood of their occurrence.
4. Genetic Factors that Influence Varicose Veins
4.1 Family History
One of the primary genetic risk factors for varicose veins is a family history of the condition. If your parents or close relatives have varicose veins, you are more likely to develop them too. This familial link highlights the role of inherited genetic variations in the susceptibility to varicose veins.
4.2 Genetic Mutations
Certain genetic mutations have been identified as potential contributors to varicose veins. These mutations can affect the structure and function of the veins, making them more prone to dilation and dysfunction. Researchers continue to investigate specific genes and their variants that may be associated with varicose veins.
4.3 Collagen Deficiency
Collagen is a vital protein that provides structural support to blood vessels. Genetic variations that result in collagen deficiency or abnormalities can weaken vein walls, making them less resilient and more susceptible to dilation. Collagen-related genetic factors can contribute to the development of varicose veins.
5. Genetic Predisposition vs. Lifestyle Factors
It is important to note that while genetics can increase the likelihood of varicose veins, lifestyle factors can also play a significant role. Individuals with a genetic predisposition may still prevent or delay the onset of varicose veins by adopting a healthy lifestyle. Lifestyle modifications can help manage the condition effectively, even in those with a genetic risk.
6. Impact of Genetics on Vein Health
Understanding how genetics influence vein health is crucial for comprehending the link between genetics and varicose veins. Several mechanisms can contribute to the development and progression of varicose veins in individuals with genetic susceptibility.
6.1 Weakness in Vein Walls
Genetic factors can lead to structural weaknesses in the vein walls, making them more susceptible to stretching and dilation. This weakness can be attributed to collagen deficiencies or abnormalities, as mentioned earlier, compromising the integrity of the veins.
6.2 Valve Dysfunction
Genetic variations can disrupt the proper functioning of the valves within the veins. When the valves fail to close properly, blood can flow backward and accumulate in the veins, resulting in their enlargement and the formation of varicose veins.
6.3 Reduced Blood Flow
Genetic factors can also impact blood flow within the veins. Alterations in genes associated with the regulation of blood flow can lead to impaired circulation, causing blood to pool in the veins and contribute to the development of varicose veins.
7. Identifying Genetic Risk Factors
Recognizing genetic risk factors for varicose veins can help individuals make informed decisions regarding prevention and treatment. The following methods can aid in identifying genetic susceptibility:
7.1 Genetic Testing
Advancements in genetic testing have made it possible to identify specific gene variants associated with varicose veins. Genetic testing can provide individuals with valuable information about their genetic predisposition, enabling them to take proactive measures to manage the condition.
7.2 Family Medical History
A comprehensive understanding of your family medical history can also shed light on your genetic risk for varicose veins. Discussing the presence of varicose veins or other venous disorders with your relatives can help you assess your own susceptibility.
8. Prevention and Management
While genetics may play a role in the development of varicose veins, there are steps you can take to prevent or manage the condition effectively.
8.1 Lifestyle Changes
Maintaining a healthy lifestyle is crucial for reducing the impact of genetics on varicose veins. Regular exercise, maintaining a healthy weight, avoiding prolonged standing or sitting, and elevating your legs can help improve blood circulation and minimize the risk of varicose veins.
8.2 Compression Stockings
Wearing compression stockings can provide external support to the veins, enhancing blood flow and reducing discomfort. These specialized stockings apply gentle pressure to the legs, preventing blood from pooling and minimizing the appearance of varicose veins.
8.3 Medical Interventions
In cases where varicose veins cause significant discomfort or complications, medical interventions may be necessary. These interventions can range from minimally invasive procedures, such as sclerotherapy or laser treatment, to surgical interventions that remove or close off affected veins.
9. Conclusion
Genetics can indeed play a significant role in the development of varicose veins. While lifestyle factors and genetic predisposition both contribute to the condition, understanding the genetic aspects can help individuals make informed decisions regarding prevention, early detection, and management. By adopting a healthy lifestyle and seeking appropriate medical interventions when needed, individuals can effectively manage varicose veins and improve their quality of life.
FAQs
FAQ 1: Can varicose veins be completely cured?
While there is no definitive cure for varicose veins, various treatment options can effectively manage the condition, alleviate symptoms, and improve the appearance of the veins.
FAQ 2: Is surgery the only option for treating varicose veins caused by genetics?
No, surgery is not the only option. Depending on the severity and specific circumstances, minimally invasive procedures such as sclerotherapy, endovenous laser treatment, or radiofrequency ablation may be recommended.
FAQ 3: Can genetic factors be modified to prevent varicose veins?
Genetic factors cannot be modified. However, lifestyle modifications and proactive measures can help reduce the impact of genetics and minimize the risk of developing varicose veins.
FAQ 4: Are all varicose veins caused by genetics?
No, varicose veins can also be caused by lifestyle factors, such as obesity, pregnancy, prolonged sitting or standing, and hormonal changes. Genetics is one of the contributing factors, but not the sole cause.
FAQ 5: Can exercise help reduce the impact of genetics on varicose veins?
Yes, regular exercise, particularly activities that promote leg movement and improve circulation, can help reduce the impact of genetics on varicose veins. Exercise strengthens the muscles that support veins and enhances blood flow, mitigating the risk of varicose veins.