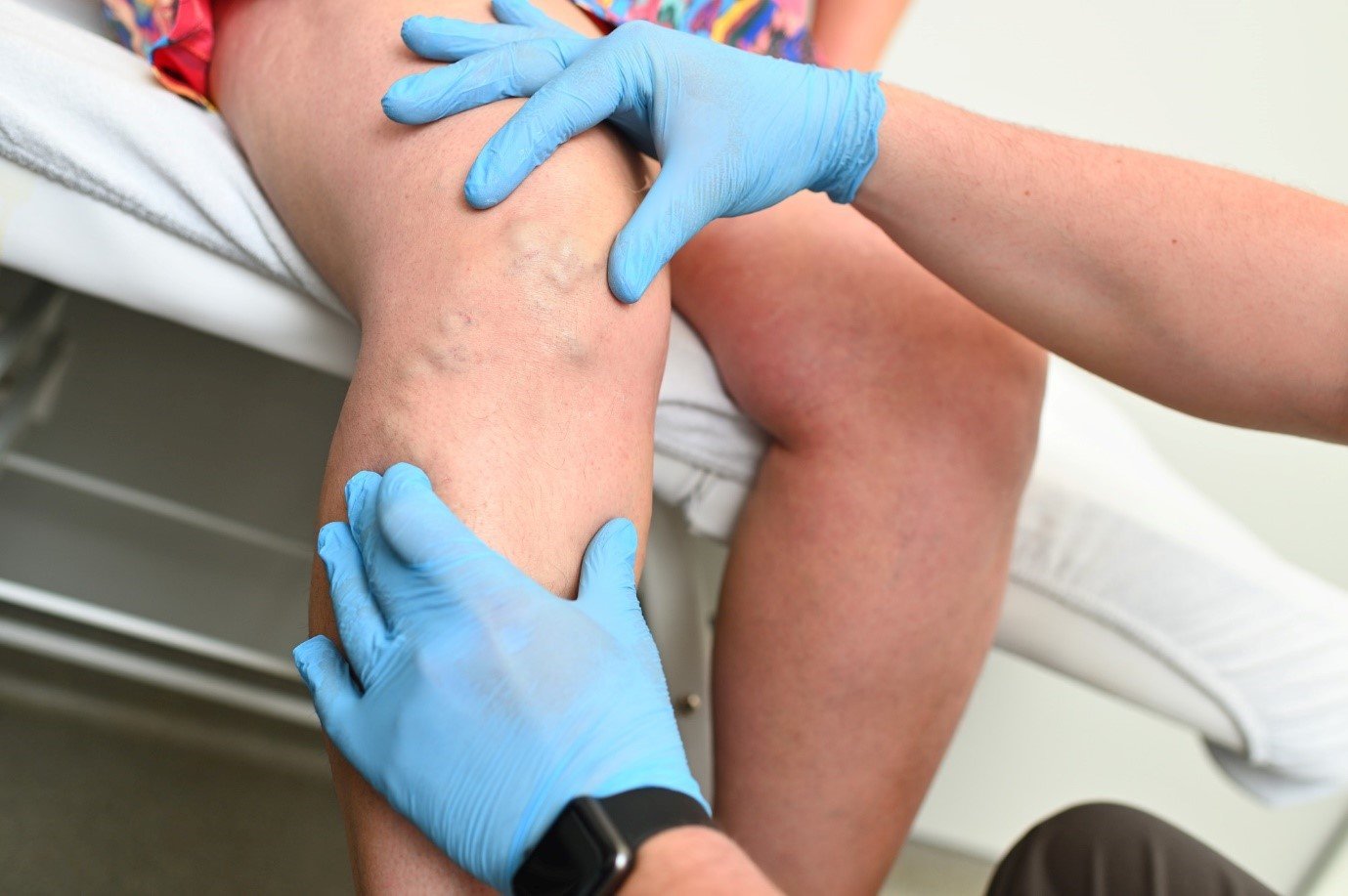
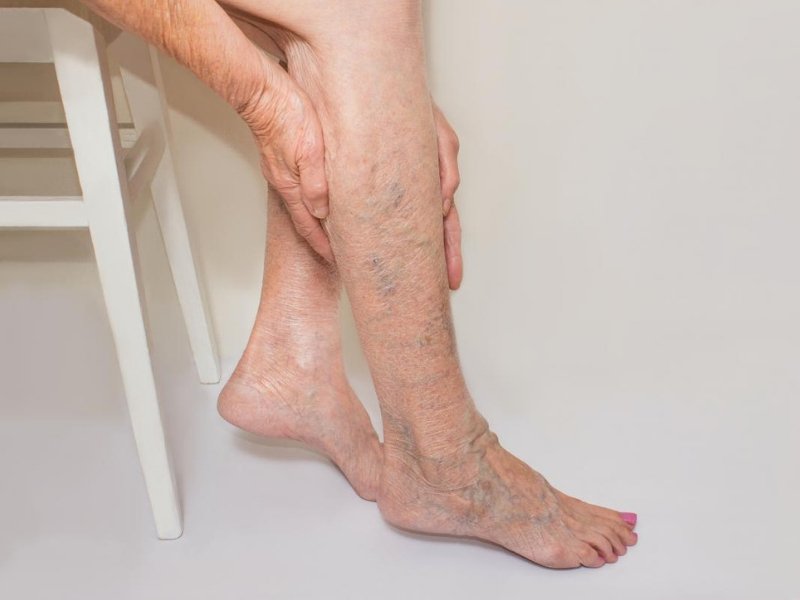
The veins in your legs carry blood back to your heart. They have one-way valves that keep blood from flowing backward. If you have chronic venous insufficiency (CVI), the valves don’t work as they should and some of the blood may go back down into your legs. That causes blood to pool or collect in the veins.
Over time, CVI can cause pain, swelling, and skin changes in your legs. It may also lead to open sores called ulcers on your legs.
Causes
A blood clot in a deep vein in your leg (called deep vein thrombosis) can damage a valve. If you don’t exercise, that can cause CVI, too. So can sitting or standing for long stretches of time? That raises the pressure in your veins and may weaken the valve.
Women are more likely than men to get CVI. Your chances also might be higher if you are:
- Obese
- Overage 50
- Pregnant or have been pregnant more than once
- From a family with a history of CVI
- Someone with a history of blood clots
- A smoker
Symptoms
-
- You may notice these in your legs
- Swelling or heaviness, especially in the lower leg and ankle
- Pain
- Itchiness
- Varicose veins (twisted, enlarged veins close to the surface of the skin)
- Skin that looks like leather
When symptoms are present the most common are heaviness or fullness, aching, restlessness, tiredness, fatigue, pain, throbbing, burning, itching and muscle cramping. In advanced cases, breakdown of the skin may cause bleeding from varicose veins, and large varicosities may develop blood clots, a condition called superficial phlebitis or thrombophlebitis. If you experience any of these symptoms, talk with your doctor. Do not ignore these symptoms.
Treatments
Most treatment is nonsurgical. The main goal is to prevent severe swelling and ulcers from developing.
- Compression garments relieve symptoms and aid ulcer healing.
- If superficial veins are affected, they may be treated through vein ablation or injection.
- If varicose veins develop and are close to the skin, they may be removed through superficial vein stripping, usually an outpatient procedure.
- If deep veins are affected, in severe cases angioplasty and stenting may be recommended.
- In rare cases, surgical bypass may be required.
Risk Factors
The most important factors leading to the development of chronic venous insufficiency and varicose veins include:
-
- Family history
- Increasing age over 30
- One or more blood clots in superficial or deep veins
- Female gender, although varicose veins occur nearly as common in men
- Multiple pregnancies
- Prolonged standing
- Heavy lifting
- Limited physical activity, high blood pressure, and obesity have also been linked with the presence of varicose veins in women
The treatment of CVI will be based on the severity of disease and guided by anatomic and pathophysiologic considerations. Compressive garments have been a mainstay in the management of CVI. Traditional surgical techniques and newer interventional methods are often reserved for an unsatisfactory response to conservative measures, although earlier use of venous ablation should be considered in symptomatic patients.